Part of our Testosterone Health Hub
Sleep is one of the most powerful and overlooked drivers of testosterone production. While diet, exercise, and supplementation can support hormonal health, the majority of daily testosterone release actually occurs during sleep.
When sleep quality declines, testosterone levels often decline as well. Research shows that even a single week of restricted sleep can significantly reduce testosterone in healthy men.
Understanding how sleep influences testosterone production—and how to improve sleep quality—can make a major difference in hormone balance, energy, libido, and overall health.
If you’re exploring the broader role hormones play in men’s health, you can start with the Complete Guide to Testosterone: Symptoms, Testing, and Natural Support.
The Connection Between Sleep and Testosterone
Testosterone production follows a circadian rhythm, meaning it rises and falls throughout the day according to the body’s internal clock.
Most testosterone is produced overnight during the first few sleep cycles.
Key facts about testosterone production during sleep include:
- Testosterone levels begin rising shortly after falling asleep
- Peak testosterone levels occur during early morning hours
- Deep sleep stages trigger the largest hormonal release
- Poor sleep reduces the total amount of testosterone produced overnight
Men who consistently sleep fewer than six hours per night often show significantly lower testosterone levels compared with men who sleep seven to nine hours.
Chronic sleep deprivation can also contribute to other hormonal disruptions, including elevated stress hormones. Learn more in High Stress and Cortisol: How They Suppress Testosterone.
How Testosterone Is Produced During Sleep
Testosterone production is controlled by the hypothalamic-pituitary-gonadal (HPG) axis.
This hormonal signaling system involves three key steps:
- The hypothalamus releases GnRH (gonadotropin-releasing hormone)
- The pituitary gland releases LH (luteinizing hormone)
- The testes produce testosterone
Sleep regulates this entire signaling chain. Deep sleep stages stimulate stronger LH pulses, which then drive testosterone production. When sleep becomes fragmented or shortened, LH signaling weakens, reducing testosterone output.
Men experiencing ongoing fatigue or hormone imbalance may also notice other warning signs. These are covered in Low Testosterone Symptoms in Men: Physical, Mental, and Sexual Signs.
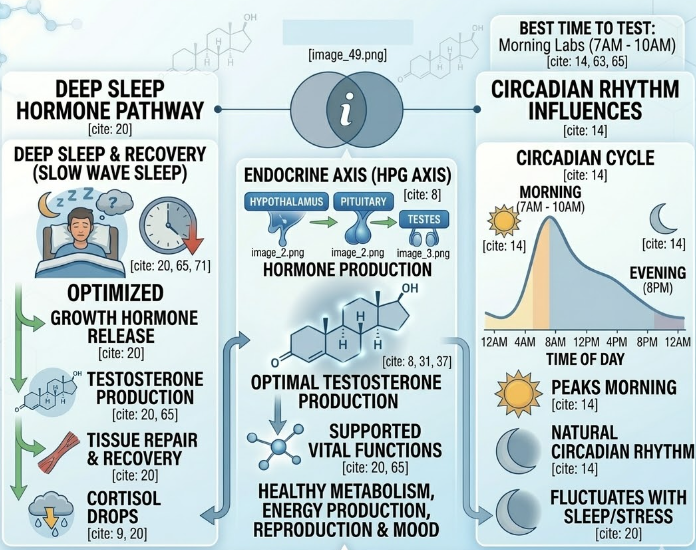
The Role of Deep Sleep (Slow Wave Sleep)
The most important sleep stage for testosterone production is deep sleep, also known as slow wave sleep. This stage typically occurs during the first half of the night.
During deep sleep:
- Growth hormone is released
- Testosterone production increases
- Tissue repair and recovery occur
- Cortisol levels drop
Deep sleep is essential for hormonal recovery and metabolic balance. Without enough deep sleep, testosterone production becomes impaired.
Because hormones affect many areas of male health, reduced testosterone can also influence sexual function and libido. Learn more in Testosterone and Erectile Function: What’s Hormonal vs Vascular.
What Happens to Testosterone When Sleep Is Restricted
Studies show that sleep restriction can reduce testosterone levels quickly. One controlled study found that healthy men who slept only five hours per night for one week experienced a 10–15% drop in testosterone levels.
Other effects of chronic sleep deprivation include:
- Lower libido
- Reduced muscle recovery
- Increased fatigue
- Higher cortisol levels
- Increased belly fat accumulation
Sleep deprivation can also worsen metabolic health and insulin resistance, which are both linked to hormonal decline. Learn more in Sugar, Insulin Resistance, and Testosterone: The Metabolic Link.
Sleep Disorders That Lower Testosterone
Certain sleep conditions are strongly linked to lower testosterone levels.
Obstructive Sleep Apnea
Sleep apnea interrupts breathing repeatedly during the night. This causes fragmented sleep and reduced oxygen levels, both of which impair testosterone production. Men with untreated sleep apnea often show:
- Lower testosterone levels
- Reduced libido
- Erectile dysfunction
- Increased fatigue
Because testosterone influences vascular health, sleep apnea is also associated with reduced sexual performance.
Insomnia
Chronic insomnia disrupts the normal sleep cycle, preventing the body from reaching deep restorative sleep stages. This leads to reduced testosterone production, elevated cortisol levels, and impaired metabolic health.
Shift Work Sleep Disorder
Men who work night shifts or rotating shifts frequently experience circadian rhythm disruption. This disrupts hormonal timing and often leads to lower testosterone levels and increased metabolic stress.
Lifestyle Habits That Improve Sleep and Testosterone
Improving sleep quality is one of the most effective ways to support natural testosterone production.
Maintain a Consistent Sleep Schedule
Going to bed and waking at the same time each day helps stabilize the circadian rhythm that regulates hormone release. Aim for 7–9 hours of sleep per night whenever possible.
Reduce Evening Light Exposure
Blue light from phones, tablets, and computers suppresses melatonin production. Reducing screen exposure before bed can improve sleep quality and hormone balance.
Avoid Late-Night Alcohol
Alcohol may initially make people feel sleepy, but it fragments sleep cycles and reduces deep sleep. This can impair testosterone production overnight. Alcohol also directly impacts testosterone levels, as discussed in Alcohol and Testosterone: What the Research Suggests.
Exercise Regularly
Regular strength training and physical activity improve sleep quality and support testosterone production. Learn more in Best Workouts for Testosterone: Strength Training Principles That Work.
Manage Stress
Chronic stress raises cortisol levels, which suppresses testosterone production and can disrupt sleep patterns.
Signs Poor Sleep May Be Affecting Your Testosterone
Men experiencing chronic sleep disruption may notice symptoms such as:
- Persistent fatigue
- Low libido
- Reduced morning erections
- Slower workout recovery
- Reduced motivation or mood changes
If symptoms persist, medical testing may help determine whether testosterone levels are affected.
When to Consider Testosterone Testing
If sleep problems and symptoms of low testosterone occur together, it may be helpful to check hormone levels. Testing is typically performed with a morning blood test, when testosterone levels are highest.
If you are considering testing, read Best Time to Test Testosterone: Morning Labs, Fasting, and Repeat Testing.
The Bottom Line
Sleep is one of the most powerful regulators of testosterone production. Most testosterone is produced during deep sleep cycles, and even short-term sleep restriction can reduce hormone levels. Improving sleep quality through consistent schedules, reduced light exposure, and healthy lifestyle habits remains a foundational pillar of testosterone health.
To explore the full topic, visit the Testosterone Health Hub.
Related Articles
- What Causes Low Testosterone?
- High Stress and Cortisol
- Best Time to Test Testosterone
- Best Testosterone Boosters
FAQ
How much sleep do men need for testosterone production?
Most research suggests that 7–9 hours of quality sleep per night is ideal for supporting healthy testosterone levels.
Does sleeping in on weekends help testosterone?
While extra rest can help with recovery, consistent sleep-wake cycles are more effective for stabilizing the circadian rhythm and hormone release.
Can sleep apnea cause low testosterone?
Yes. Sleep apnea causes sleep fragmentation and oxygen deprivation, both of which significantly impair the body’s ability to produce testosterone.
Is deep sleep the most important stage for hormones?
Yes. Most testosterone is produced during the deep, slow-wave sleep stages that typically occur in the first half of the night.
Explore the Testosterone Health Hub
Sleep is only one piece of the testosterone puzzle. Explore the full hub to learn how lifestyle, nutrition, hormones, and medical testing influence testosterone levels.
Visit the Testosterone Hub